How To Fix Plantar Fasciitis
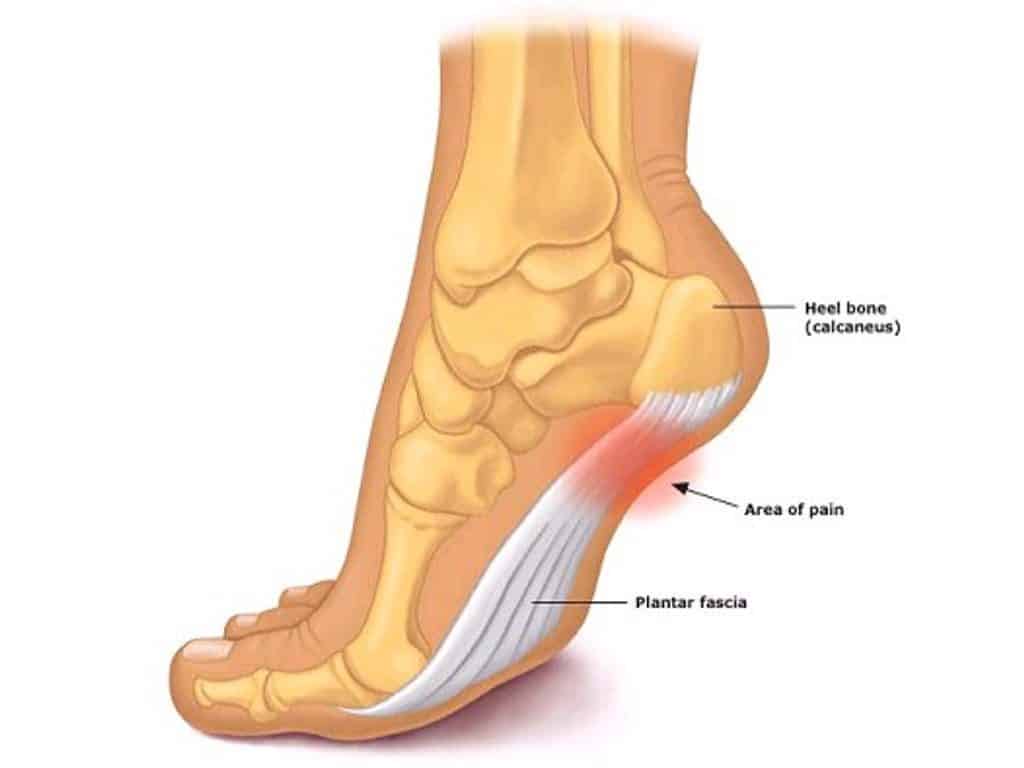
Ever wanted to learn how to treat and fix plantar fasciitis? Plantar fasciitis is a common condition that affects the foot and causes pain in the heel and sole. It occurs when the plantar fascia, a thick band of tissue that connects the heel to the toes, becomes inflamed or irritated. As a health clinic, it is essential to have a comprehensive management plan to help patients manage their pain and return to their normal activities. Here are some of the best management guidelines for plantar fasciitis.
Education
Education is the foundation of managing plantar fasciitis. Patients should be educated about the causes of plantar fasciitis and how to avoid them. The main causes of plantar fasciitis are;
- Overuse or excessive physical activity: Repetitive activities that put stress on the plantar fascia, such as running, jumping, or standing for long periods, can lead to inflammation and microtears in the tissue, resulting in plantar fasciitis.
- Foot mechanics and abnormalities: Abnormal foot mechanics, such as flat feet (pronation) or high arches (supination), can alter the distribution of weight and strain on the plantar fascia, increasing the risk of injury and inflammation. Structural abnormalities like leg length discrepancies and tight calf muscles may also contribute.
- Improper footwear: Wearing shoes that lack proper arch support or cushioning, or shoes that don’t fit properly, can place excessive stress on the plantar fascia and contribute to its inflammation. High heels and flip-flops are examples of footwear that can exacerbate the condition.
- Obesity: Excessive body weight can increase the strain on the plantar fascia, leading to inflammation and pain.
- Age: Plantar fasciitis is more common in middle-aged individuals, typically between 40 and 60 years old. This may be due to the natural aging process, which can result in decreased flexibility and elasticity of the plantar fascia.
- Certain occupations and activities: Jobs or activities that involve prolonged standing or walking on hard surfaces, such as factory workers, teachers, or athletes, can increase the risk of developing plantar fasciitis.
- Pre-existing medical conditions: Certain medical conditions, such as rheumatoid arthritis, spondyloarthritis, lupus, and diabetes, can be associated with an increased risk of plantar fasciitis.
Patients should also be informed about the importance of proper footwear, stretching, and strengthening exercises.
Manual therapy
Manual therapy can help reduce pain and improve function in patients with plantar fasciitis. Techniques such as soft tissue mobilization, myofascial release, and trigger point therapy can be used to release tension in the plantar fascia and surrounding muscles. Make sure to see your physiotherapist, massage therapist or naturopathic doctor for help in this matter.
Stretching
Stretching exercises can help improve flexibility and reduce pain in patients with plantar fasciitis. Specific stretches for the plantar fascia and calf muscles can be prescribed to patients to perform at home. Again, please see your therapist for direction in stretching for your condition.
Strengthening
Strengthening exercises can help improve the strength of the muscles in the foot and ankle. Strengthening exercises for the intrinsic foot muscles, calf muscles, and hip muscles can be prescribed to patients to perform at home or in the clinic. Each patient is different and it is always important to have a full assessment done by a qualified therapist.
Here is an example of one of our favourite exercises to improve mobility and stability in the foot for patients with Plantar Fasciitis. Credit for this video goes out to PhysioTutors.
Orthotics
Orthotics, such as arch supports or shoe inserts, can be used to support the foot and relieve pressure on the plantar fascia. Custom orthotics can be prescribed to patients based on their individual needs.
Taping
Taping techniques can be used to support the foot and reduce tension on the plantar fascia. Techniques such as low-dye taping and kinesiology taping can be used to provide support and reduce pain.
Modalities
Modalities such as ultrasound, electrical stimulation, and ice can be used to reduce pain and inflammation in patients with plantar fasciitis.
Conclusion
By implementing education, manual therapy, stretching, strengthening, orthotics, taping, and modalities, patients can achieve successful outcomes. It is important to individualize treatment plans to meet the specific needs of each patient. Please make sure to reach out to professional to diagnose and help treat your condition.
Also see; Treating Tennis Elbow
References
- Riel H, Cotchett M, Delahunt E, Rathleff MS, Vicenzino BT, Weir A, Landorf KB. Is ‘plantar heel pain’ a more appropriate term than ‘plantar fasciitis’? Time to move on. Br J Sports Med. 2017 Jun;51(11):1576-1577. doi: 10.1136/bjsports-2016-096981. Epub 2017 Jan 24. PMID: 28119364.
- McClinton SM, Heiderscheit BC, McPoil TG. Plantar fasciitis: clinical practice guidelines linked to the international classification of function, disability, and health from the orthopaedic section of the American Physical Therapy Association. J Orthop Sports Phys Ther. 2008 Aug;38(8):A1-A18. doi: 10.2519/jospt.2008.0305. PMID: 18678962.
- Riddle DL, Schappert SM. Volume of ambulatory care visits and patterns of care for patients diagnosed with plantar fasciitis: a national study of medical doctors. Foot Ankle Int. 2004;25(5):303-310. doi:10.1177/107110070402500507
- Wearing SC, Smeathers JE, Urry SR, et al. Plantar fasciitis: are pain and fascial thickness associated with arch shape and loading?. Phys Ther. 2007;87(8):1002-1008. doi:10.2522/ptj.20060255
- Cole C, Seto C, Gazewood J. Plantar fasciitis: evidence-based review of diagnosis and therapy. Am Fam Physician. 2005;72(11):2237-2242. PMID: 16342847.
- Riddle DL, Pulisic M, Pidcoe P, Johnson RE. Risk factors for plantar fasciitis: a matched case-control study. J Bone Joint Surg Am. 2003;85(5):872-877. doi:10.2106/00004623-200305000-00015.